Transcatheter Pulmonary Artery Stenosis Treatment
Stenosis of the pulmonary arteries may be congenital or postoperative, and may lead to right ventricular hypertension and hypertrophy and ultimately significant cardiac dysfunction.
When pulmonary artery stenosis is diagnosed in the first few months of life, the usual treatment is transcatheter balloon angioplasty.
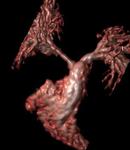
MRI imaging of a patient with pulmonary artery stenosis
If stenosis occurs after the first 18 months of life, it is possible in the majority of cases, to implant a stent in the lumen of the vessel to keep it open, hence open heart surgery may be avoided.
Before the stent placement, you will be asked to perform an MRI or CT scan to assess the exact dimensions and anatomy of the vessel. Occasionally, particularly if recent diagnostic catheterization has been preceded, no further imaging is required prior to the interventional procedure.
Once the CT or MRI confirms that stent implantation is feasible and appropriate measurements are made to assess the degree of stenosis, we perform a cardiac catheterization, usually through the patient’s groin.
The procedure is performed under general anesthesia.
Injection of contrast media is performed in the right ventricle and the pulmonary arteries to assess the diameter of maximum stenosis, as well as the diameter of the healthy vessel parts beyond, and therefore select the appropriate balloon / stent size.
There are several types of stent that can be used, depending on the age of the child and anatomy of the vessels (picture).
Stenosed vessel
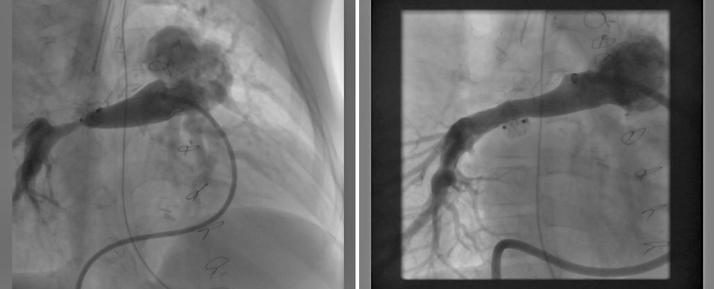
Following stent implantation
After implantation, the patient stays in the hospital for 1-2 days. A Chest X-ray and an echocardiogram are performed before discharge.
The only medication given after the procedure is aspirin, which is continued for up to 6 months after stent implantation.

